
Your body aches. You lose friends. Kids grow up and leave home. Loved ones pass away. You grapple with loneliness. Time seems to be speeding up – and you may feel powerless to stop it.
But, it’s not all bad news. According to The United States of Aging Survey, seniors are more optimistic than ever:
-
- More than 8 in 10 agree with the statement “I have a strong sense of purpose and passion about my life and my future.”
- Nearly two thirds of respondents (65 percent) say the past year of their life has been normal or better than normal.
- More than 3 in 4 seniors aged 60 to 69 expect their quality of life to stay the same or get better over the next 5 to 10 years.
If 75 percent of seniors expect their quality of life to stay the same or improve, it indicates that they are not just feeling good physically – they are feeling good mentally. One way to maintain a good mental quality of life is to seek appropriate treatment for depression.
Treating depression in patients 65 years and older can be different than treating younger patients. Age, the presence of other illnesses, and other medications you may be taking are three factors that your doctor may take into consideration when treating depression.
Age Can Affect Medication Decisions
Aging may impact how patients process certain medications. The FDA states:
“As you get older, body changes can affect the way medicines are absorbed and used. For example, changes in the digestive system can affect how fast medicines enter the bloodstream. Changes in body weight can influence the amount of medicine you need to take and how long it stays in your body. The circulatory system may slow down, which can affect how fast drugs get to the liver and kidneys. The liver and kidneys also may work more slowly, affecting the way a drug breaks down and is removed from the body.”
Age can also complicate genetic factors. Older patients may have impaired production of CYP450 enzymes, which can affect drug metabolism rate, according to an article published in Current Medicinal Chemistry.
How Other Illnesses Can Impact Depression Treatment

And these conditions may bring on depression. According to the National Institute of Mental Health (NIMH), people with other chronic medical conditions have a higher risk of depression. Further, “research suggests that people who have depression and another medical illness tend to have more severe symptoms of both illnesses.”
Depression shouldn’t be dismissed as just another part of illness. It can and should be treated. Talking with your doctor about your other illnesses is an important part of your treatment.
“You should also inform the healthcare provider about all treatments or medications you are already receiving, including treatment for depression (prescribed medications and dietary supplements),” writes the NIMH. “Sharing information can help avoid problems with multiple medications interfering with each other. It also helps the provider stay informed about your overall health and treatment issues.”
Managing Multiple Medications in Depression Treatment
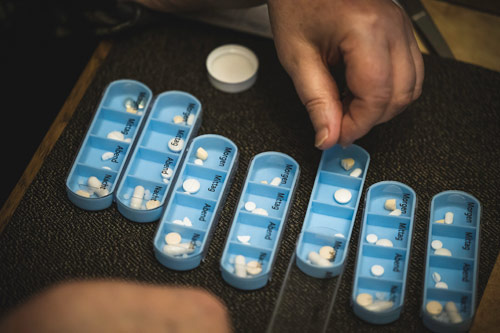
“Many of the patients who come to see me for treatment of depression, for example, are on multiple other medicines. Cardiac medicines, medicines for pulmonary disease, medicines for pain, chronic osteoarthritis is a very common presentation for many of my patients,” said Dr. Allan Anderson, a specialist in geriatric psychiatry and past president of the American Association of Geriatric Psychiatry. “It’s uncommon for me to have any geriatric patients that come in not on any medication.”
Patients are often seeing various specialists for differing ailments. As a result, since no single provider is responsible for managing the patient’s complete medication profile, drug/drug interactions could occur.
This can lead to adverse drug reactions. According to an article by the American Family Physician, “adverse drug events occur in 15 percent or more of older patients presenting to offices, hospitals, and extended care facilities. These events are potentially preventable up to 50 percent of the time.”
What to Expect when Talking with Your Doctor
The first step in getting a depression diagnosis is scheduling an appointment with your doctor.
Often, the clinician will start by using a diagnostic depression screening tool. There is a depression rating scale developed specifically for screening for depression in older adults called the Geriatric Depression Scale Short Form (GDS-SF).
This 15-item screening tool typically takes 5-7 minutes to administer and asks questions like if the patient is “satisfied” with their life, if they feel their life is empty, or if they often get bored. If the doctor believes depression is present, he or she will determine an appropriate treatment, which may include talk therapy, antidepressant medication, or other therapies.
For more information about the types of antidepressant medications, please read our blog post.
Our articles are for informational purposes only and are reviewed by our Medical Information team, which includes PharmDs, MDs, and PhDs. Do not make any changes to your current medications or dosing without consulting your healthcare provider.
The GeneSight test must be ordered by and used only in consultation with a healthcare provider who can prescribe medications. As with all genetic tests, the GeneSight test results have limitations and do not constitute medical advice. The test results are designed to be just one part of a larger, complete patient assessment, which would include proper diagnosis and consideration of your medical history, other medications you may be taking, your family history, and other factors.
If you are a healthcare provider and interested in learning more about the GeneSight test, please contact us at 855.891.9415. If you are a patient, please talk with your doctor to see if the GeneSight test may be helpful.




